OPRA™ Implant System
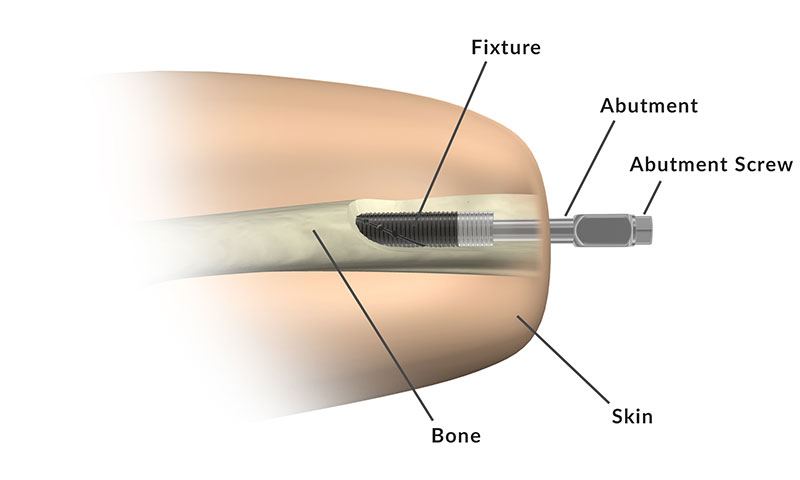
The OPRA™ Implant System is a bone anchored system based on osseointegration where the prostheses are directly attached to the bone and thus avoiding the use of socket. The system utilizes a modular design consisting of three main parts that have been developed and refined over the years based on many years of development and clinical research. The unique design ensures protection of the patient by avoiding bone fractures from accidental loads. The implant components are inserted surgically into the bone of the amputation stump in one or two surgical sessions.
- Fixture: Anchoring element inserted into the patient’s bone
- Abutment: Skin penetrating connection attached to the fixture
- Abutment Screw: A screw made of titanium alloy that locks the Abutment to the Fixture

OPRA™ Fixture BioHelix™
Improved osseointegration
A new surface technology has been introduced (BioHelix™), after 15 years of research and clinical testing. The new surface will take osseointegration to the next level and promote faster, stronger attachment to bone, thereby increasing the strength of the bone-to-implant interface
It started already in 2004 when Integrum´s unique BioHelix™ surface was developed in close collaboration with the Department of Biomaterials at the University of Gothenburg. Since then, several experimental studies have shown more rapid healing and stronger osseointegration.
Features of the OPRA™ Fixture BioHelix™
- Decreased time to healing and improved bone-to-implant stability
- Increased degree of osseointegration, created by its micro- and nano-sized structures that takes osseointegration to the next level
- Significantly increased strength of the bone-to-implant interface (proven in several studies)
A well proven system used in over 500 surgeries
The OPRA™ Fixture is coated with a new surface technology, BioHelix™, that has been developed by Integrum after 15 years of research and clinical testing. The surface will take osseointegration to the next level and promote faster, stronger attachment to the bone, thereby increasing the strength of the bone-to-implant interface. The prosthesis is connected to the OPRA™ Implant System using a connection, load controlling device. Integrum has developed specific components each customized for different indication levels, including both upper and lower limb.
The OPRA™ Implant System components are implanted during one or two surgeries. The first surgery with the OPRA™ Implant System was performed in 1990 by Professor Per-Ingvar Brånemark and Professor Björn Rydevik and over the coming almost 30 years, more than 500 surgeries have been performed in fourteen countries. Clinical studies show that the surgery significantly improves the quality of life for amputees.

Benefits
- Increased range of motion
- Eliminates pressure, sores and pain caused by the socket
- Stable attachment
- Easy attachment and detachment
- Better walking ability
- Improved osseoperception (sensory feedback)
- Can be worn all day, every day
- Improved sitting comfort
- No socket adjustments required
- Suitable for short amputation stumps
Prosthesis
The abutment is connected to the external prosthesis through different safety devices, depending on the amputation level. The prosthetic components include attachment, alignment and load control functions designed to protect the implant from accidental loads. Below you find the specific prosthetic components for amputations above the knee, along with an information video.
Proven in Clinical Studies
Prospective study in 51 transfemoral amputees with the OPRA™ Implant System. The cumulative fixture survival rate at 5 years was 92%, and the revision-free survival rate was 45%. Thirty-four patients had 70 superficial infections. Eleven patients had 14 deep infections. Fifteen patients had mechanical complications. Four fixtures were removed (ie, one deep infection and three loosening). Patient-reported (PRO) outcome measures showed significant improvements including more use of the prosthesis, better mobility, fewer issues, and improved physical health-related quality of life (all P < 0.0001) compared with baseline. Conclusion: Individuals with TFA at 5-year follow-up had significant improvement in PRO measures, but increases in deep infections and mechanical complications are concerning. Results from in-depth interviews reported by Lundberg, Hagberg & Bullington (2011)2 showed that patients using a bone-anchored prosthesis experienced a revolutionary change that went beyond the functional gains, to improve quality of life. One of the patients expressed this in the following way:
“The other prosthesis ruled my life, it was my master in a way, it’s inevitable…it affected my mood and my interest in doing things that I knew would demand an extra effort. You had to weigh the pros and cons and that’s all gone now. Now it’s actually me…I am in command and not the left leg (socket prosthesis) and that’s a big difference.”
1Brånemark, R., Hagberg, K. Kulbacka-Ortiz, K., Berlin, Ö., Rydevik, B. (2018). Osseointegrated percutaneous prosthetic system for the treatment of patients with transfemoral amputation: A prospective five-year follow-up of patient-reported outcomes and complications. J Am Acad Orthop Surg, doi: 10.5435/JAAOS-D-17-00621
2Lundberg, M., Hagberg, K., & Bullington, J. (2011). My prosthesis as a part of me: a qualitative analysis of living with an osseointegrated prosthetic limb. Prosthet Orthot Int, 35(2), 207–14
Patient Information Video
Are You a Potential Candidate?
Are you an amputee who experiences problems with conventional socket prostheses? Then the OPRA™ Implant System may be applicable for you.
